Smaller and newer Medicare Advantage (MA) plans face an uphill climb in the Stars program. Limited resources, lean teams, and evolving infrastructure make high performance hard to sustain. Yet, these same plans have unique advantages: speed, agility, and closeness to their members and provider partners.
This article distills actionable lessons from Lilac’s recent webinar covering how smaller and newer MA plans can punch above their weight class and outperform in Stars. Our learnings come from years of hands-on experience in Stars operations, compliance, and technology innovation. The webinar (recording above) and this article are designed to help Stars leaders at smaller and newer plans not only compete but win in an increasingly challenging Stars environment.
Understanding the Performance Curve
Data across the MA landscape shows clear performance patterns by both plan size and plan age.
Key Findings Based on Plan Size
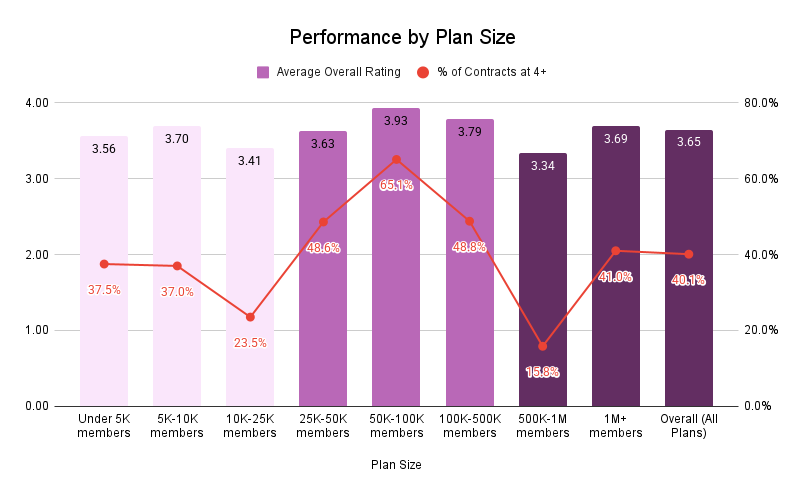
- Small plans (under 25k members) tend to be the lowest performers on average.
- Mid-sized plans (25k–500k members) is the highest performing segment, with enough resources to invest in organizational and technology infrastructure and the agility to move fast.
- Large plans (500k+ members) are middle performers on average with a few national plans seeing regression in a significant portion of contracts.
Key Findings Based on Plan Age
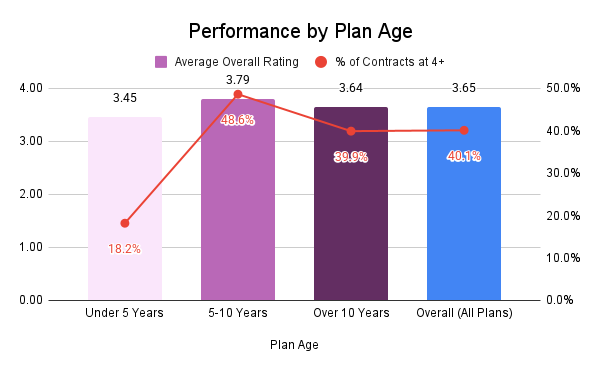
- Young plans (under 5 years) struggle the most with an average Star rating of 3.45, which is largely a product of resources and program maturity.
- Middle aged plans (5-10 years) by far perform the best as they tend to have the best balance of maturity and innovation.
- Older plans (over 10 years) have scores above the younger plans but below the middle-aged plans, which might indicate challenges associated with organizational ossification.
Lesson 1: Strengthen Your HEDIS Vendor Partnership
Your HEDIS vendor relationship can be a big needle mover in your plan’s Star performance. For smaller plans, the right data cadence and transparency are what you need to establish quickly.
What to Expect from Your Vendor
- Frequent data runs: Demand monthly or quarterly runs and not just annual snapshots.
- Minimal data lag: Faster cycles enable real-time interventions.
- Granular reporting: Ensure access to subpopulation and equity-level breakdowns to support EHO4All calculations.
Plans relying solely on year-end reports are too late to act. The best-performing smaller plans treat their HEDIS vendor as a strategic partner to engage continuously, not a compliance function to engage transactionally.
Lesson 2: Use Agentic AI to Expand Member Engagement Capacity
Smaller teams are closer to members but still face challenges engaging every member for every care gap, medication need and staying in tune with satisfaction levels. The challenges lie in orchestration and thoughtfully orchestrating all types of outreach for maximal impact without risking abrasion. This is where agentic AI can be a difference maker.
AI powered systems now allow plans to:
- Reliably merge data from scattered spreadsheets into one unified member profile.
- Generate personalized outreach recommendations based on member history and overlapping measures.
- Automate voice, SMS, or email outreach across all parts of the risk spectrum, which frees up human staff for higher-touch engagement.
In short: Agentic AI isn’t a replacement. It’s a multiplier!
Lesson 3: Make CAHPS and HOS a Central Pillar
Member experience measures are no longer “soft” metrics. They now carry significant weight – up to 25% of overall Stars scores when combined.
Where to Focus
- Ownership: Assign clear responsibility for CAHPS and HOS performance.
- Continuous feedback: Use pulse surveys and micro-feedback loops to detect member sentiment early.
- Engage the “neutral middle”: Identify and follow up with members who rate you 6s and 7s, not just the extremes.
- Track wellbeing trends: Use claims, case management, and social data to identify members with declining health or mobility before survey season.
Small plans have the proximity and personal relationships to outperform on these measures. They just need systematic tracking and tools for continuous engagement.
Lesson 4: Manage PBMs Like a Strategic Extension of Your Team
PBMs vary dramatically in how much Stars support they provide. Smaller plans often get less attention. Proactivity (and pushiness) matters.
The Best PBMs Offer
- Near real-time adherence tracking (daily or weekly).
- Predictive risk scoring to identify members likely to become noncompliant.
- Root-cause analysis for why gaps occur and how to close them.
- PDE reconciliation to catch CMS errors that can cost you points.
If your PBM can’t deliver this level of support, supplement with analytics tools that do. Lilac has built out a full suite of medication adherence and drug measure modules to help in this mission critical area.
Lesson 5: Track Operational Measures Daily
Operational metrics like appeals, call center response, and CTMs are highly sensitive for small plans. Just a few errors can cost a star.
Best Practices
- Daily monitoring: Treat every case as critical.
- Early auditing: Fix pharmacy and PDE data before CMS deadlines.
- Plan preview review: Recheck for misclassified calls, appeals, and CTMs.
- Scenario modeling: Stay ahead of potential CMS measure changes and their impact on total Stars scoring.
Operational precision is one of the few areas where small plans can outperform much larger peers through vigilance and speed.
Lesson 6: Stay Ahead of CMS and Market Changes
Stars is evolving faster than ever—with new measures, weighting shifts, and equity adjustments. Successful smaller plans are those that plan forward, not react backward.
- Model Stars scenarios annually to understand how new measures or weighting will impact your contract.
- Pilot future measures early, especially HEDIS updates and polypharmacy metrics.
- Integrate real-time forecasting tools to identify where to invest resources before cut points are finalized.
Agility isn’t just an advantage. It’s your moat.
Lesson 7: The Bottom Line: Small, Smart, and Strategic Wins
Stars excellence for smaller and newer MA plans isn’t about scale. It’s about precision, speed, and member focus.
Winning plans:
- Start Stars management from day one.
- Build real-time visibility into every measure.
- Use Agentic AI to extend limited staff capacity.
- Treat satisfaction and engagement as core operational priorities.
- Audit relentlessly and fix errors early.
- Adapt faster than the competition.
With the right data foundation and modern automation, small plans can outperform at any scale. Smaller and newer plans have a distinct opportunity to transform agility into their most powerful competitive advantage.
———————————————–
Lilac has deep expertise in helping smaller and newer plans leapfrog the maturity curve through AI powered technology. Reach out here to start a conversation with the Lilac team about how we can help your plan.