The Stars data seem to show that there is a learning curve in Star and bigger is not always better.
A great deal of focus on the Medicare Advantage (MA) Stars front has been on the plight of the largest plans when it comes to quality achievement. Star ratings collectively peaked in 2022 as COVID flexibilities were in place in terms of measure and rating calculations. In the three Star years following, collective Star ratings plummeted. In Star Year 2026, we see stability but not really recovery. So, slightly positive news, but not really good news.
But what does the data tell us about the other 25% of enrollment in regional and smaller plans?
Lilac looked at Star Year 2026 results from two perspectives – tenure of contracts (not organizations per se) and size of contract membership. It tells an interesting story – that regional plans have higher ratings than the largest ones and that as plans age in the MA program and grow, Stars achievement increases.
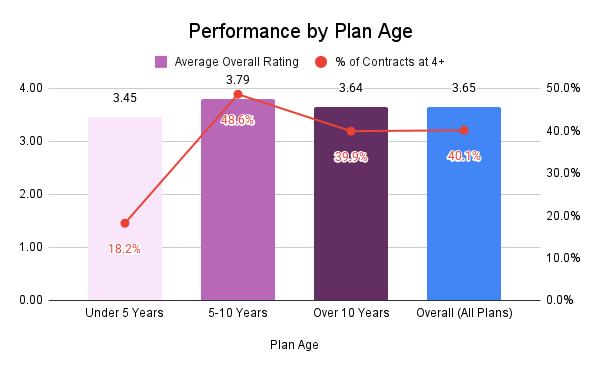
Let’s look first at tenure. It stands to reason that newer plans know less about Stars when they start and gain knowledge of best practices over time. Thus, plans under five years tend to have fewer high performing plans – just 18.2% in SY 2026 had ratings of 4 Star and greater. (Admittedly, the 3.5 Star default rating in the first few years impacts the calculation a bit). But the data show that as plans enter the 5-to-10-year tenure category, the Star rating increases dramatically – 48.6% of contracts had ratings of 4 Star or greater. This compares to 40.1% of all contracts.
There is even reason to believe that tenure above 10 years might breed a bit of complacency as just 39.9% of contracts hit 4 Star and greater. Some of this could be influenced by poor large player performance right now but the statistics over time seem to bear out this tenure-complacency factor.
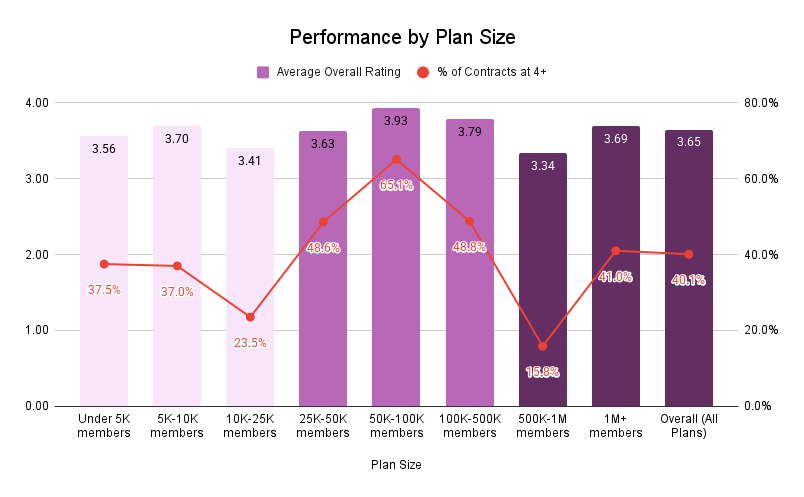
So, let’s turn to contract size. We see a similar pattern emerge – medium-sized MA contracts tend to perform best. Contracts between 50K and 100K have a 4 Star or greater rating percentage of 65.1%, with contracts between 25K and 50K enrollment at 48.6% and plans between 100K and 500K enrollment at 48.8%. The average overall ratings for these groupings also are among the highest with a few exceptions at the bottom and top.
Now, when the largest players perform well, they tend to have 4 Star and greater contract enrollment percentages that rival the mid-size plans. But that there is inconsistency for the biggest contracts points to another factor beyond tenure complacency that may influence achievement. As the organization gets bigger and bigger, additional complications of ensuring the highest performance emerge. Challenges with disparate data, a lack of agility to respond to clinical changes, and a lack of connectivity with members and providers seem to emerge. An argument could be made that decentralizing Stars administration could offset these barriers in big organizations, but that in and of itself breaks critical coordination and standardization needed to ensure consistent performance.
What does all this tell us?
First, the sweet spot for size may be in the middle and bigger is not always better. Medium-sized plans appear to have the sophistication to succeed and the important connectivity to members and providers needed to monitor and drive results.
Second, while newer plans and smaller plans initially struggle, they do learn and adapt over time. Most of them graduate and become the sophisticated medium-sized plans in the middle in terms of tenure and size.
So, the future may very well lie in the middle. While big plans dominate enrollment right now, their penetration has dropped every so slightly of late, signaling a potential shift in the MA market. All plans need to improve quality achievement, but the data show a compelling business proposition for MA generally for new entrants and regional players. At the same time, the growing complexity of Star is not for the faint of heart. Sophistication, agility, and resiliency will always be key to consistently high Star performance.
Lilac Software can help you build that sophistication, agility, and resiliency. Learn more about our best-practice approach to Stars data, forecasting and improvement – backed by the power of agentic AI here.
Or reach out here to start a conversation to discuss how we can your plan.